-

Kenya’s healthcare workers abuse a third of teen mums from informal settlements – study
Anthony Idowu Ajayi, African Population and Health Research Center and Caroline W. Kabiru, African Population and Health Research Center Adolescent pregnancy is a global public health concern: in 2022, about 13% of girls and young women gave birth before the age of 18. Compared with women in their early 20s, adolescents are more susceptible to…
-
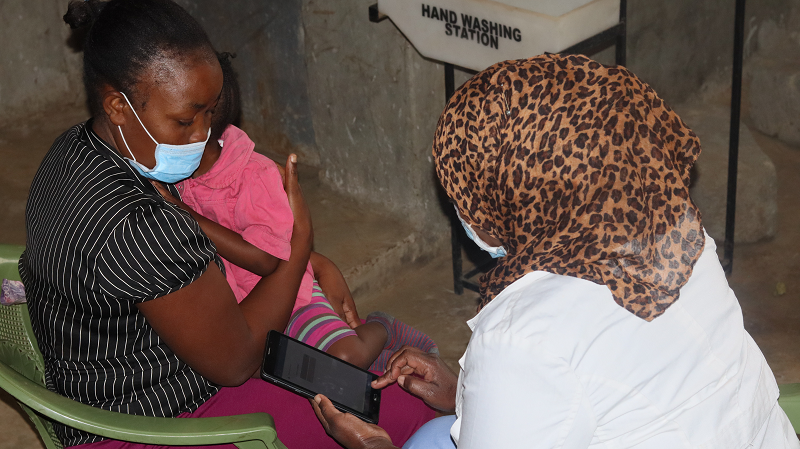
How health workers in Kibera are assessing sick children using a new digital health tool
By Maryanne W. Waweru l maryanne@mummytales.com Nairobi, Kenya, East Africa. After two days of nursing her two-year-old daughter at home, an anxious Maximilla Kangahi made her way to a clinic in her neighbourhood for help. At the health facility, Maximilla was received by Waida Kasaya, clinical officer at the Beyond Zero clinic in Karanja, one of Kibera’s 18…
-

Yes, Kenya’s Election Had Problems, But Here’s Why Things Are Better
Contributed by Hillary Omala, the Executive Director of CFK Africa Fifteen years ago, more than 1,100 people lost their lives in the violence following Kenya’s 2007 elections. Every five years since then, the Kenya General Elections have occupied international headlines, and tensions have risen across the country as painful memories come flooding back. But the…
-

Saving lives with medical oxygen in Kenya
For Sandra Karimi, a nurse at Wangige Hospital in Kenya, treating patients during the COVID-19 pandemic felt like working in a war zone.
-

Gender Equality Is Imperative to Reach Sustainable Development Goals
In 1994, governments, advocates, health organizations, women’s and youth activists gathered in Cairo for the International Conference on Population and Development (ICPD). There, women’s reproductive health and rights took center stage in national and global development efforts. This year marks the 25th anniversary of the ICPD and a renewed emphasis on reproductive health, women’s empowerment…
-
BioLite Brightens East Africa One Home at a Time
I have visited enough traditional family huts and homes in rural Africa to know that light and power are precious commodities. When the last bit of sun streams through the windows and doors in the evenings, the only recourse for light again is when the sun shines brightly in the morning. That is a long…
-
Kenya’s Marie Stopes ban may drive more women to unsafe abortions
According to the Kenya Medical Practitioners and Dentists Board, they banned abortion services provided by Marie Stopes following complaints from the general public. Restrictive laws mean that women resort to unsafe means. jbdodane/Flickr Michael Mutua, African Population and Health Research Center The Kenyan Medical Practitioners and Dentists Board has stopped the NGO Marie Stopes International from performing…
-
Suffering in silence: how Kenyan women live with profound childbirth injuries
Shutterstock Kathomi Gatwiri, Southern Cross University Sasha is 22-years-old. She was married off when she was just nine and by the time she was 11, she was pregnant with her first child, and unprepared for childbirth. So when labor came, in the middle of the night – in her geographically isolated village in rural Kenya…
-
Kenya Maternity Fee Waiver is Great – But There are Still Gaps in the Policy
Kenya’s pregnancy policy hasn’t addressed the inequalities between rich and poor. Shutterstock Estelle Monique Sidze, African Population and Health Research Center About 21 pregnant women die every day in Kenya due to complications from childbirth. That’s equivalent to two 10-seater commuter micro minibuses, known as matatus, crashing every day with the loss of all the…
-

Why Kenya Needs to Adopt ‘Milk Banks’ to Reduce Infant Deaths
Elizabeth Kimani-Murage, Brown University Mother’s milk has an enormous impact on child survival. While in Kenya it has improved over the past decade, the number of children who die before five years remains significant. The rate has decreased from 115 per 1000 live births in 2003 to 52 in 2014. Neighbors Rwanda (2008), Tanzania (2012)…
-
How a Breastfeeding Initiative in Rural Kenya Changed Attitudes
Exclusive breastfeeding is recommended up to 6 months of age. Alissa Everett/Reuters Judith Kimiywe, Kenyatta University and Elizabeth Kimani-Murage, Brown University There’s a growing global recognition of proper infant nutrition in the child’s first 1000 days of life. This can be monitored through encouraging proper nutrition during pregnancy and the first two years of life…
-
Ensuring Safer Pregnancies for Kenyan Women in Urban Slums
Antenatal care is important during pregnancy. Reuters Blessing Mberu, African Population and Health Research Center; Kanyiva Muindi, African Population and Health Research Center, and Patricia Elungata, McGill University Globally, there’s a general decline in the number of women who die from pregnancy or childbirth complications. However in Kenya, it remains high at 488 deaths per…
-

Impress Mom With These Maternal Health Mother’s Day Gift Ideas + Giveaway
Mother’s Day is the perfect holiday to splurge on the moms in your life as well as to support moms around the world. It’s a day to show love for mothers we know and to also remain mindful of the mothers everywhere who may need a little or even a lot of help for them…
-
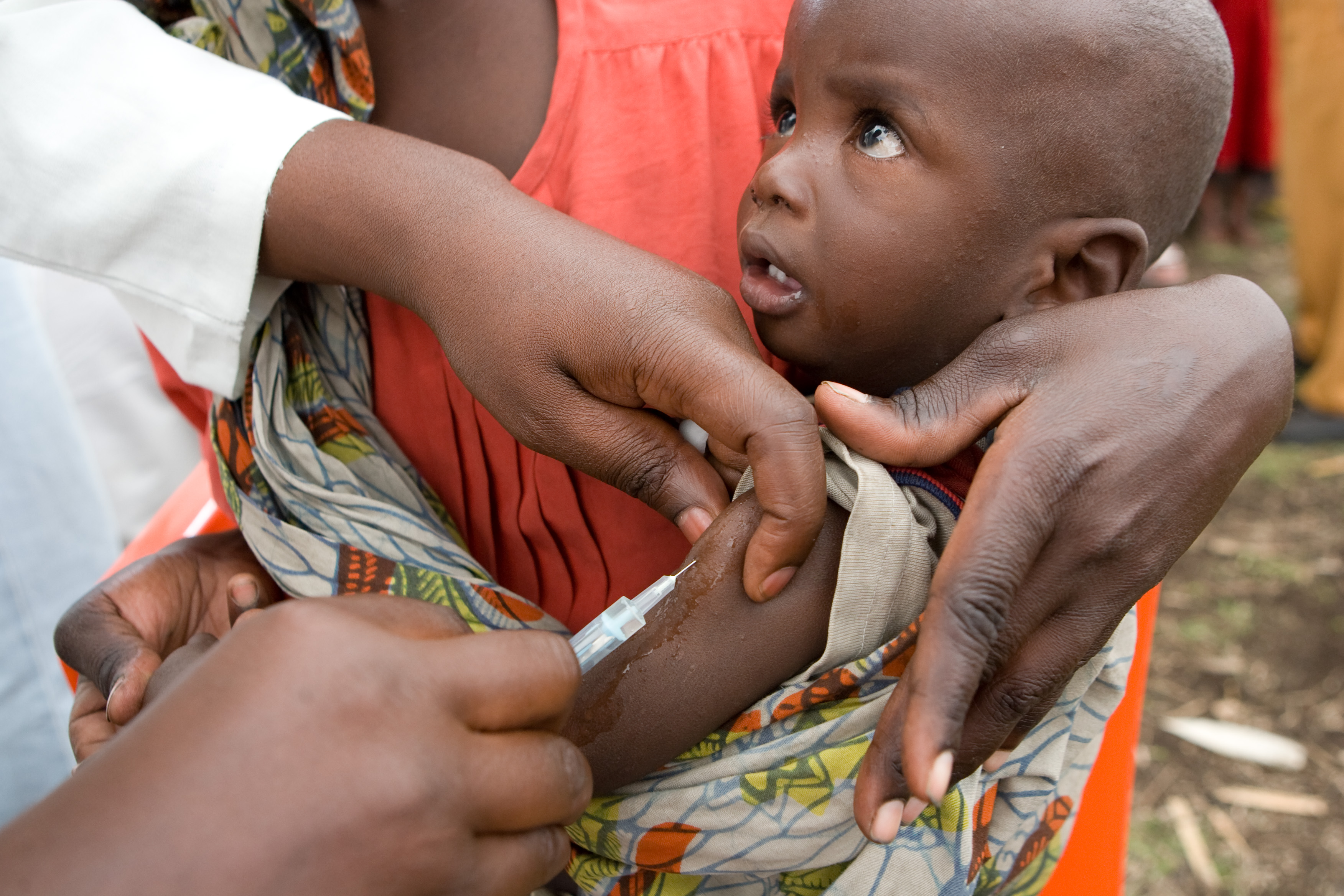
Three African Countries Chosen for First Malaria Vaccine Trials
For decades, there has been consistent chatter, research, and hope for a potential malaria vaccine. Now, all three are finally coming to fruition to roll out the world’s first clinical malaria vaccine trials. The World Health Organization Regional Office for Africa (WHO/AFRO) announced today that Ghana, Kenya, and Malawi have been chosen for the WHO-coordinated pilot…
-

Kenya is a Breastfeeding Success Story But Still Has Its Challenges
By Elizabeth Kimani-Murage, Brown University Breastfeeding has both short-term and long-term nutritional benefits for children. Nutrition is central to sustainable development. Good nutrition in the first 1000 days of a child’s life is critical for child growth, well being and survival, and future productivity. The World Health Organisation recommends exclusive breastfeeding for children until they are six…
-

Renewable Energy Company Commits to Providing Two Million Solar Kits to Kenyans
As of 2014 only 23% of Kenyans have access to electricity according to the World Bank. That number has remained steady since 2005. Now, a reported two million Kenyans will gain access to renewable energy through portable home solar kits donated by renewable energy company, US-based SkyPower. The home kits will include LED bulbs, a fan,…
-

New Global Grant Improves Obstetric Surgical Safety in Western Kenya
Earlier this week we wrote that Duke University researchers discovered that spinal anesthesia (epidurals) can be given to women during C-sections in low-resource settings in Ghana. Now, there is even more good news regarding women in Africa who are in need of emergency C-sections during high-risk deliveries. Vanderbilt University Medical Center (VUMC), Kenya’s AIC Kijabe Hospital,…
-

New Global Projects Measure Newborn Health Interventions #EveryNewborn
Eight million children under the age of five die every year from preventable diseases. Of those eight million deaths, 2.8 million are neonates according to the World Health Organization. Key interventions like Kangaroo Mother Care, pre-and postnatal care, deliveries in a hospital setting with trained health workers, and exclusive breastfeeding are some proven ways to keep more babies alive.…
-
Turkana Children in Kenya Continue to Suffer Malnutrition Amid Poor Health Services
Last week, I travelled from the capital city of Nairobi, Kenya, to Turkana County which is in the northern part of the country. Turkana is a largely pastoralist community with a population of 855,000 people. The county faces major problems, chief among them recurring droughts which has for years crippled the county’s economic development. The…
-
Exclusive Breastfeeding Rates in Kenya Still Low
By Maryanne W. Waweru, Kenyan motherhood blogger and maternal/child health journalist based in Nairobi. As Kenya joins the rest of the world in marking the World Breastfeeding Week, health experts in the country are calling on more stringent efforts to be put in place that will encourage more women to exclusively breastfeed their babies. Though…
