-

Aid Cuts Could Result in A Child Under Five Dying Every Forty Seconds by 2030, Says Oxfam
One of Oxfam’s latest reports says that a child under five may die every forty seconds by 2030 due to these drastic cuts to humanitarian aid. This is especially heartbreaking as global humanitarian efforts have saved more newborn and child lives, and the data proves it.
-

Billions of dollars, decades of progress spent eliminating devastating diseases may be lost with undoing of USAID
For over 50 years, researchers, clinicians and policymakers in the global health community have worked to eliminate infections, but the gutting of USAID could undo everything.
-

Book Review: No Woman Left Behind
No Woman Left Behind: A Journey of Hope to Heal Every Woman Injured in Childbirth by Kate Grant My rating: 5 of 5 stars No Woman Left Behind: A Journey of Hope to Heal Every Woman Injured in Childbirth is a powerful and deeply moving memoir by Kate Grant, founding CEO of the Fistula Foundation.…
-

The Most Dangerous Place to Give Birth in the World and Four Ways You Can Help
Despite decades of progress in global health, pregnancy and childbirth remain life-threatening events for millions of women, especially in the world’s most fragile settings.
-

New Law Bans Child Marriage in Sierra Leone
Photo by Majkl Velner on Unsplash This month Sierra Leone banned child marriage and laid out severe punishments for those engaging in marrying girls and boys off before their 18th birthday. 30 percent of girls in Sierra Leone are married before 18. More girls can focus on furthering their education instead of starting families at…
-

Baylor University Conducts In-Person, Virtual Training to Save Mothers, Babies
Baylor College of Medicine has performed substantive work in The Gambia to instruct frontline health workers on maternal and child health through its “Training of Trainers” and GOALL (Gambian Obstetrics Anesthesia Learning and Leadership) programs. With the ninth-highest maternal mortality rate, access to quality health care for women of reproductive age in The Gambia is…
-

Kenya’s healthcare workers abuse a third of teen mums from informal settlements – study
Anthony Idowu Ajayi, African Population and Health Research Center and Caroline W. Kabiru, African Population and Health Research Center Adolescent pregnancy is a global public health concern: in 2022, about 13% of girls and young women gave birth before the age of 18. Compared with women in their early 20s, adolescents are more susceptible to…
-

Nonprofit Works to Eradicate Poverty Through Business, Not Charity
I have had the pleasure of reporting from low-income countries in east Africa, Asia, and the Caribbean many times and have seen a multitude of poverty eradication efforts from organizations that are created by social entrepreneurs to those that are funded by foundations, corporations and countries’ developmental aid. No matter the organizations’ efforts, there are…
-
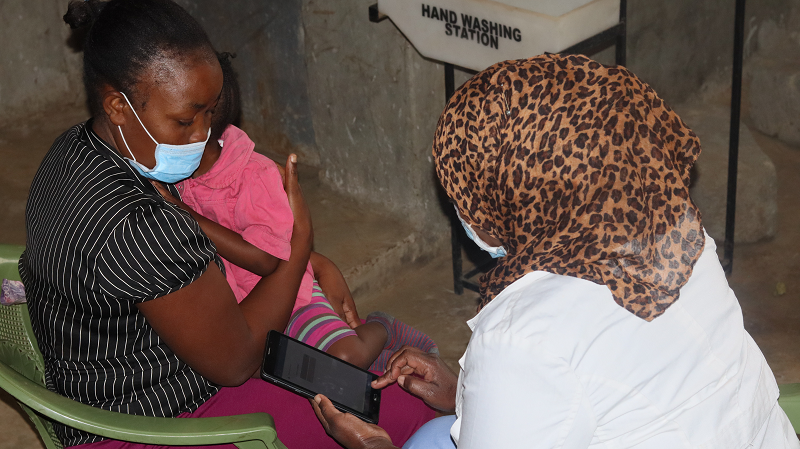
How health workers in Kibera are assessing sick children using a new digital health tool
By Maryanne W. Waweru l maryanne@mummytales.com Nairobi, Kenya, East Africa. After two days of nursing her two-year-old daughter at home, an anxious Maximilla Kangahi made her way to a clinic in her neighbourhood for help. At the health facility, Maximilla was received by Waida Kasaya, clinical officer at the Beyond Zero clinic in Karanja, one of Kibera’s 18…
-

Yes, Kenya’s Election Had Problems, But Here’s Why Things Are Better
Contributed by Hillary Omala, the Executive Director of CFK Africa Fifteen years ago, more than 1,100 people lost their lives in the violence following Kenya’s 2007 elections. Every five years since then, the Kenya General Elections have occupied international headlines, and tensions have risen across the country as painful memories come flooding back. But the…
-

Saving lives with medical oxygen in Kenya
For Sandra Karimi, a nurse at Wangige Hospital in Kenya, treating patients during the COVID-19 pandemic felt like working in a war zone.
-
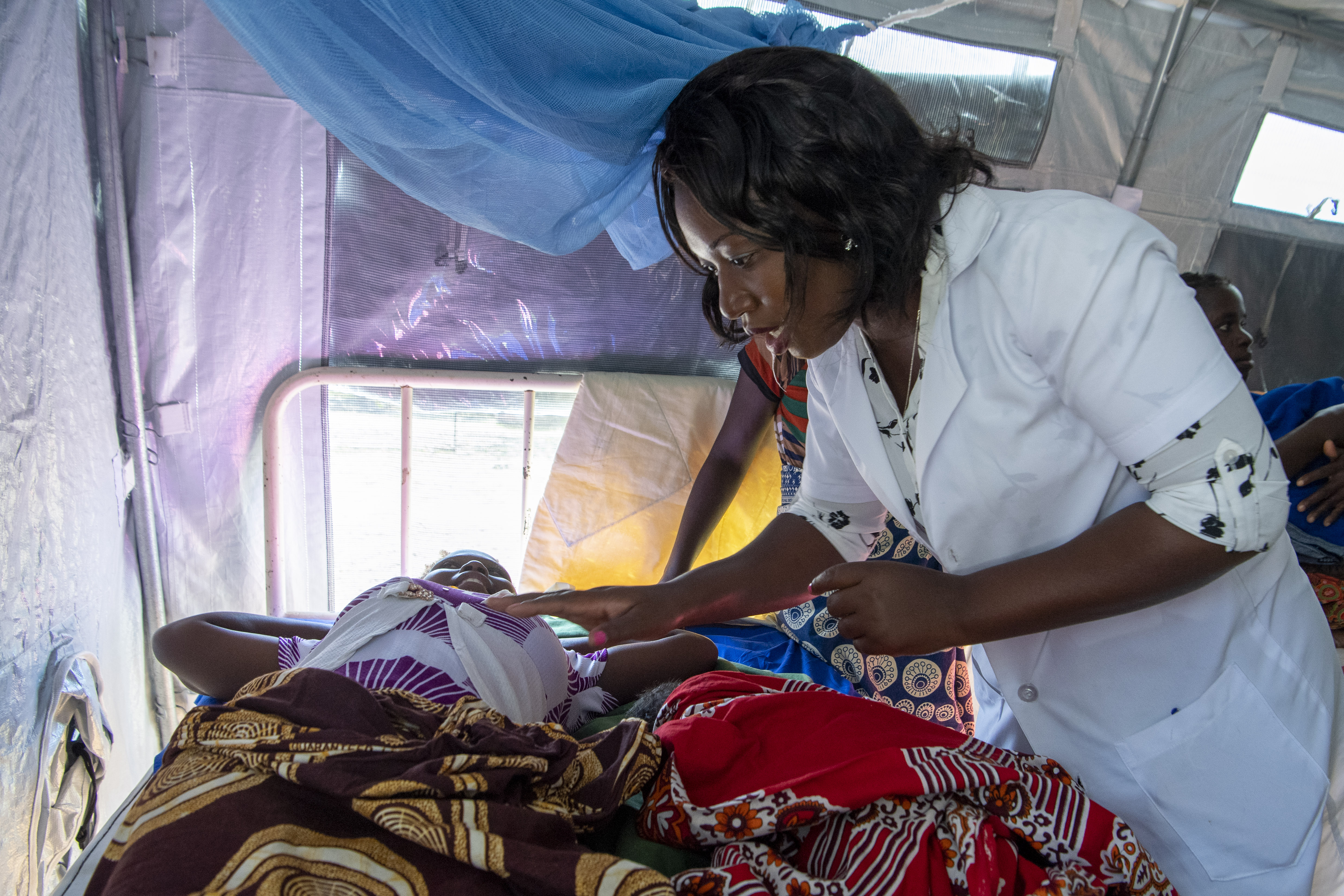
Why sexual and reproductive law for east African countries is being resisted
Anthony Idowu Ajayi, African Population and Health Research Center and Nicholas Okapu Etyang, African Population and Health Research Center Six of the countries of the East African Community – Burundi, Kenya, Rwanda, South Sudan, Uganda and Tanzania – recently concluded public hearings on a new sexual and reproductive health bill. Proponents of the bill argue…
-

On This #IWD2022 Join CAMFED’s Global Sisterhood to Educate Young Girls
CAMFED is one the world’s leading organizations that advocates for and helps young girls in sub-Saharan Africa attain an education. CAMFED which stands for the Campaign for Female Education has to date supported 379,000 young girls with secondary school scholarships, one million girls attend primary school, and works with 6,787 partner schools across sub-Saharan Africa.…
-

Poor knowledge and practice around oxytocin could put women in Nigeria at risk during childbirth
Chioma S. Ejekam, University of Lagos and Chimezie Anyakora, Pan Atlantic University Severe bleeding after childbirth – postpartum hemorrhage – is a leading cause of maternal morbidity and mortality in middle-income countries. Oxytocin is an affordable and effective drug that’s recommended to prevent postpartum hemorrhage. But there are concerns about the quality of oxytocin available…
-

Ethiopia’s Tigray Region Is still Under Attack
If you have followed my travels or have read my blog over the years you know that Ethiopia is my favorite country in the world. There is something about the people, the culture, its beauty and the sheer size of the country I love. Even though I love Ethiopia I have never been under a…
-

The Universal Human Right to an Identity from Birth Explained
By Caroline Kinsella, Advocacy and Communications Intern, White Ribbon Alliance One of the more hidden human rights abuses around the world is the fact that one billion people have no legal proof of identity. Alarmingly, UNICEF estimates that about one in four children under age 5, or 166 million, are unregistered and without any trace…
-
[WATCH] Video Shows Horrors of Childbirth in Sierra Leone #MaternalHealth
The United Nations has designated Sierra Leone as the most dangerous place to have a baby. In fact, it has the highest maternal mortality rate in the world at 1,360 deaths per 100,000 live births. On average, most women have at least six babies in Sierra Leone. In a previous post I mentioned the Aminata…
-

Radiotherapy will be required to treat cervical cancer in low-and-middle income countries
When I was in Zambia I saw ways in which nurses treat cervical cancer in low resource settings. Women who do not benefit from the HPV vaccine and still develop cervical cancer are often subject to visual inspection of the cancer typically with a digital camera followed by cryotherapy to freeze the diseased part of…
-
NEW: Drug That Prevents PostPartum Hemorrhage Added To WHO Essential Medicines List
As I have written many times before postpartum hemorrhage (PPH) or excessive uterine bleeding after childbirth is the leading cause of maternal mortality in low-and-middle income countries. The recommended drug to prevent PPH according to the World Health Organization (WHO) is oxytocin. When administered in its recommended dose it causes little to no side effects.…
-

Netflix Movie Reveals Grim Reality of Nigeria to Europe Sex Trafficking
Tens of thousands of young Nigerian girls and women leave their country every year with sincere hopes of starting a brand-new life in Europe where they believe they will be met with ample job and educational opportunities to provide for their families. That is what they are often told by “recruiters” in their home states…
