-
BioLite Brightens East Africa One Home at a Time
I have visited enough traditional family huts and homes in rural Africa to know that light and power are precious commodities. When the last bit of sun streams through the windows and doors in the evenings, the only recourse for light again is when the sun shines brightly in the morning. That is a long…
-
Kenya’s Marie Stopes ban may drive more women to unsafe abortions
According to the Kenya Medical Practitioners and Dentists Board, they banned abortion services provided by Marie Stopes following complaints from the general public. Restrictive laws mean that women resort to unsafe means. jbdodane/Flickr Michael Mutua, African Population and Health Research Center The Kenyan Medical Practitioners and Dentists Board has stopped the NGO Marie Stopes International from performing…
-
Suffering in silence: how Kenyan women live with profound childbirth injuries
Shutterstock Kathomi Gatwiri, Southern Cross University Sasha is 22-years-old. She was married off when she was just nine and by the time she was 11, she was pregnant with her first child, and unprepared for childbirth. So when labor came, in the middle of the night – in her geographically isolated village in rural Kenya…
-
Kenya Maternity Fee Waiver is Great – But There are Still Gaps in the Policy
Kenya’s pregnancy policy hasn’t addressed the inequalities between rich and poor. Shutterstock Estelle Monique Sidze, African Population and Health Research Center About 21 pregnant women die every day in Kenya due to complications from childbirth. That’s equivalent to two 10-seater commuter micro minibuses, known as matatus, crashing every day with the loss of all the…
-

Why Kenya Needs to Adopt ‘Milk Banks’ to Reduce Infant Deaths
Elizabeth Kimani-Murage, Brown University Mother’s milk has an enormous impact on child survival. While in Kenya it has improved over the past decade, the number of children who die before five years remains significant. The rate has decreased from 115 per 1000 live births in 2003 to 52 in 2014. Neighbors Rwanda (2008), Tanzania (2012)…
-
How a Breastfeeding Initiative in Rural Kenya Changed Attitudes
Exclusive breastfeeding is recommended up to 6 months of age. Alissa Everett/Reuters Judith Kimiywe, Kenyatta University and Elizabeth Kimani-Murage, Brown University There’s a growing global recognition of proper infant nutrition in the child’s first 1000 days of life. This can be monitored through encouraging proper nutrition during pregnancy and the first two years of life…
-
Increasing Caesarean Sections in Africa Could Save More Mothers’ Lives
Shutterstock Salome Maswime, University of the Witwatersrand and Gwinyai Masukume, University of the Witwatersrand Caesarean sections have been lifesaving procedures for hundreds of thousands of women across the world who experience complications during labour. Globally, it’s estimated that just under 20% of births take place via caesarean section – a percentage that’s gone up over…
-

5 Maternal Health Interventions That Save Mothers’ Lives
Every day 800 women die during childbirth or from pregnancy complications. This startling statistic represents women who not only live in sub-Saharan Africa where most maternal deaths occur but also throughout the world. In order to reduce the number of maternal deaths in low- and middle-income countries across the globe design teams, social entrepreneurs, innovators, and…
-

To Empower Women, Give Them Better Access to Water
Bethany Caruso, Emory University Imagine going through your day without ready access to clean water for drinking, cooking, washing or bathing. Around the world, 663 million people face that challenge every day. They get their water from sources that are considered unsafe because they are vulnerable to contamination, such as rivers, streams, ponds and unprotected…
-

Announcing #MaternalHealthChat Starting November 8 With Jacaranda Health
We are very pleased and excited to announce our new weekly chats all about maternal health with some of the leading maternal health experts, researchers, practitioners, and organizations in the world under the #maternalhealthchat hashtag. Starting on Tuesday, November 8 at 1 PM EST with Jacaranda Health we will host 30-minute chats each week all about maternal and reproductive health…
-

Better Maternal Care in Africa Can Save Women from Suffering in Childbirth
Kareemah Gamieldien, Cape Peninsula University of Technology Every year just over 500,000 women die from complications in pregnancy and childbirth across the world. Another 20 million experience severe complications. But many of these complications are entirely avoidable – including obstructed and protracted labour and one of its side-effects, obstetric fistula. An obstetric fistula is a…
-

Why Mothers Aren’t Accessing Antenatal Care Early in Their Pregnancies
Anja Smith, Stellenbosch University South Africa has extremely high maternal mortality levels. This is true when compared with developed countries as well as other developing countries. According to the World Health Organisation, for every 100,000 live births in the country in 2015, 138 women died due to pregnancy and childbirth complications. In Sweden, fewer than…
-
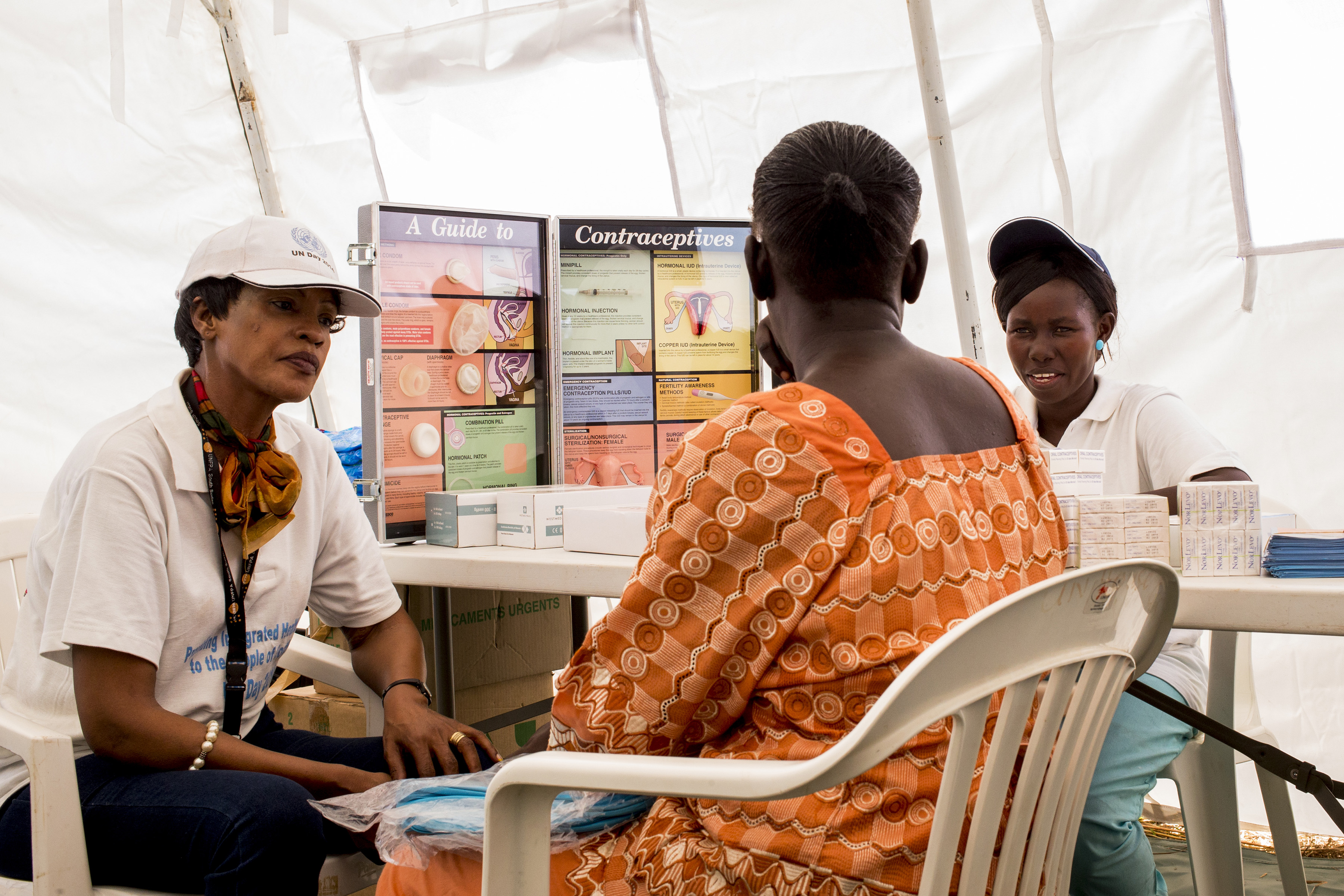
Why a new vaginal ring could be a game-changer in HIV prevention
Thesla Palanee-Phillips, University of the Witwatersrand The results of the two studies showing that a vaginal ring can help reduce the risk HIV infection among women is being hailed as an important HIV prevention breakthrough. Launched four years ago, the two clinical trials, known as ASPIRE and The Ring Study, set out to determine how…
-

What’s Driving sub-Saharan Africa’s Malnutrition Problem?
Sub-Saharan Africa has the highest level of food insecurity in the world. An estimated 220 million people lack adequate nutrition. The nature of the problem is shifting rapidly, with overweight status and obesity emerging as new forms of food insecurity while malnutrition persists. But continental policy responses do not address this changing reality.
-

Photo Essay: Standing in Line for Voluntary Male Circumcision
Over the past decade there has been growing research that purports the long-held belief that Voluntary Medical Male Circumcision (VMMC) can drastically decrease the rates of HIV, sexually transmitted diseases, and urinary tract infections in low-and middle-income countries. In Tanzania, for example, where these photos were taken at an IntraHealth International mobile clinic, HIV can…
-

West Africa Declared Ebola Free, Despite Recent Outbreak
For two years Ebola has drastically ravaged three West African countries – Sierra Leone, Guinea and Liberia – and has taken the lives of 11,300 people according to the Guardian UK. Over 28,000 people were diagnosed with Ebola and still live with the pain and stigma of the disease. Since Liberia has not reported a…
-
![Maternal Health Around the World [Infographic]](https://socialgoodmoms.com/wp-content/uploads/2015/11/651340.jpg)
Maternal Health Around the World [Infographic]
Brought to you by Nursing@Georgetown: Nurse Midwife programs Photo: United Nations
-

Only a Global Response Can Solve Europe’s Refugee Crisis
Phil Orchard, The University of Queensland The recent deaths of asylum seekers attempting to reach European shores have prompted ongoing calls for action. But, given the scale of the issue, only a comprehensive, global program can go some way to solving the crisis. The UN High Commissioner for Refugees (UNHCR) notes that more than 366,000…
-

Maternal Health Heroes: Interview With Liya Kebede #MHHSS
We are excited to publish our fourth interview in our Maternal Health Heroes Summer Series with Liya Kebede, Supermodel and Founder of the Liya Kebede Foundation. Throughout the summer we will speak with some of the most notable maternal health advocates in the world ahead of the Global Maternal Newborn Health Conference that will be held in Mexico City between October 18 – 21,…

