-

Aid Cuts Could Result in A Child Under Five Dying Every Forty Seconds by 2030, Says Oxfam
One of Oxfam’s latest reports says that a child under five may die every forty seconds by 2030 due to these drastic cuts to humanitarian aid. This is especially heartbreaking as global humanitarian efforts have saved more newborn and child lives, and the data proves it.
-

Free Guide for Members: How to Use Your Voice to Advocate for Change
Influence for Good: How to Use Your Voice to Advocate for Change shares practical strategies for using social media to raise awareness, build meaningful connections, and advocate for causes that truly matter, especially for women, families, and communities often left out of the conversation.
-

Baylor University Conducts In-Person, Virtual Training to Save Mothers, Babies
Baylor College of Medicine has performed substantive work in The Gambia to instruct frontline health workers on maternal and child health through its “Training of Trainers” and GOALL (Gambian Obstetrics Anesthesia Learning and Leadership) programs. With the ninth-highest maternal mortality rate, access to quality health care for women of reproductive age in The Gambia is…
-
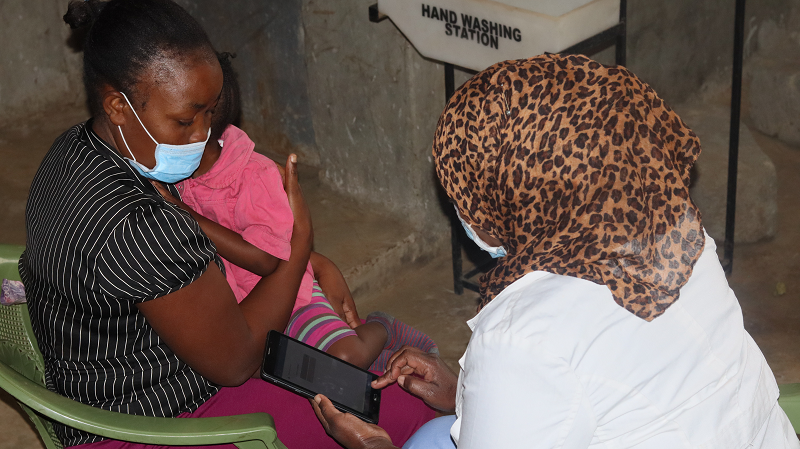
How health workers in Kibera are assessing sick children using a new digital health tool
By Maryanne W. Waweru l maryanne@mummytales.com Nairobi, Kenya, East Africa. After two days of nursing her two-year-old daughter at home, an anxious Maximilla Kangahi made her way to a clinic in her neighbourhood for help. At the health facility, Maximilla was received by Waida Kasaya, clinical officer at the Beyond Zero clinic in Karanja, one of Kibera’s 18…
-

First Malaria Vaccine Rolls Out in Malawi
It is heartening to see progress in the fight against malaria. Over the past thirty years and with hundreds of millions of dollars invested thus far, the RTS,S malaria vaccine was officially rolled out yesterday in Malawi. In 2017, I wrote about the vaccine trials that began in 2009 and the announcement of the three countries…
-

January Is Birth Defects Prevention Month: Are Local Health Departments Ready?
Q&A with NACCHO Board Member Sandra Elizabeth Ford, MD, MPH Director of the DeKalb County Board of Health A baby is born with a birth defect in the United States every 4.5 minutes, according to the Centers for Disease Control and Prevention (CDC). Birth defects are defined as any structural changes present at birth that…
-

Can Fitbit Help Kids Gain Steps and Lose Weight?
Around 17 percent of American children from age 2 to 19 are classed as “obese”. That’s a level that has remained fairly steady over the last decade. And it’s growing. Obesity is measured in terms of Body Mass Index (BMI) – a measure that can be used to compare children in terms of their weight.…
-

How World Vision Promotes Breastfeeding in the Philippines
I am always happy when World Breastfeeding Week rolls around each year. It gives me a chance to hear about the latest programs that are working around the world to increase breastfeeding rates. This year I learned about how World Vision is promoting breastfeeding in the Philippines through its 7-11 Core Intervention Framework which includes 7 interventions for women…
-
How a Breastfeeding Initiative in Rural Kenya Changed Attitudes
Exclusive breastfeeding is recommended up to 6 months of age. Alissa Everett/Reuters Judith Kimiywe, Kenyatta University and Elizabeth Kimani-Murage, Brown University There’s a growing global recognition of proper infant nutrition in the child’s first 1000 days of life. This can be monitored through encouraging proper nutrition during pregnancy and the first two years of life…
-

Why 20 Million People Are on the Brink of Starvation and How You Can Help
It’s difficult to fathom that 20 million people are on the brink of starvation in Sub-Sharan Africa and the Middle East, but the statistic is true. In fact, the region is facing the largest humanitarian crisis in over seventy years and if no help is provided 1.4 million children are at risk of death. Not…
-
[Featured Video] Simple Birth Kit for Mothers in Developing World
Women in low-and-middle-income countries need clean birth kits in order to stave off deadly infections in themselves and their newborns. This is the case not only during home births with midwives but also in institutionalized settings. Zubaida Bai, founder of Ayzh, a social enterprise that creates clean, safe birthing kits for women as well as reproductive, newborn…
-
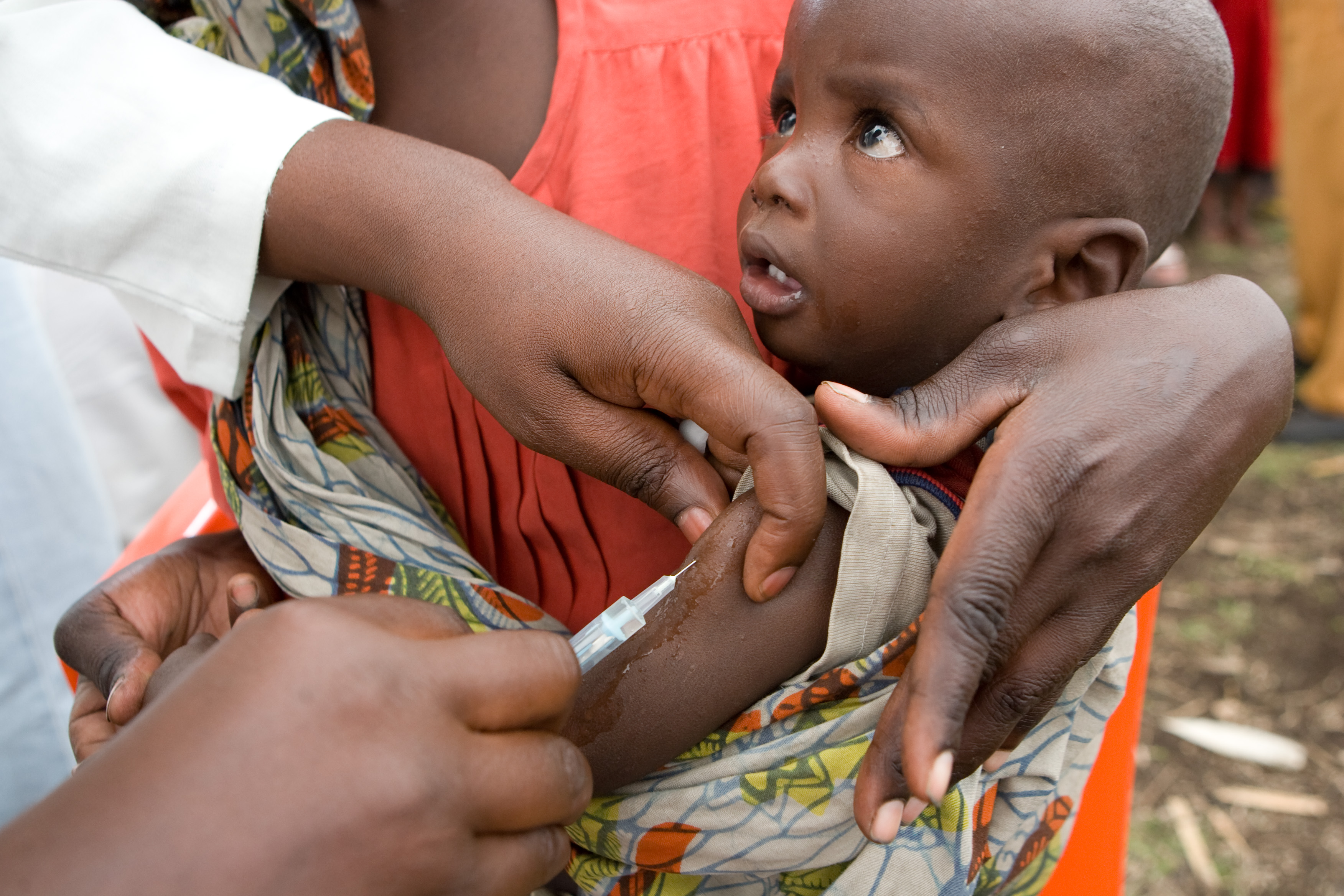
Three African Countries Chosen for First Malaria Vaccine Trials
For decades, there has been consistent chatter, research, and hope for a potential malaria vaccine. Now, all three are finally coming to fruition to roll out the world’s first clinical malaria vaccine trials. The World Health Organization Regional Office for Africa (WHO/AFRO) announced today that Ghana, Kenya, and Malawi have been chosen for the WHO-coordinated pilot…
-

How You Can Help Mothers and Babies in Syria’s Idlib Camps
War is suffocating every corner of Syria and has been for the past several years. In areas that are close to neighboring countries like Idlib province that borders Turkey, Syrians from all over the country are fleeing there for safety believing that those border regions won’t fall under severe air attack. Unfortunately, as we learned…
-

Residents in Southern Haiti Receive New Access to Quality Health Care
During my visit to Haiti two years ago I had the privilege of visiting two hospitals: L’Hôpital Albert Schweitzer (HAS) in Haiti’s Artibonite Valley and L’Hôpital Sainte-Thérèse in Hinche, Haiti. Many of the patients at both hospitals, I learned, walked or took public transport over long distances for quality hospital care. As the poorest country in the…
-

Double Your Donation Today By Giving to World Vision #GivingTuesday
When I travel to low-income countries I am most interested in learning about and reporting on maternal and newborn health. As a mother of two daughters it is my biggest passion. Today on Giving Tuesday I am proud to work with one of my favorite international nonprofit organizations: World Vision USA. I had the distinct opportunity…
-

Maternal Malnutrition Affects Future Generations: Kenya Must Break the Cycle
By Elizabeth Echoka, Kenya Medical Research Institute and Lydia Kaduka, Kenya Medical Research Institute Nutrition of women before and during pregnancy and when breastfeeding is critical in determining the health and survival of the mother and of her unborn baby. Undernourished pregnant women have higher reproductive risks. They are more likely to experience obstructed labour, or…
-

Where Have 4.8 Million Syrian Refugees Gone?
Jeffrey H. Cohen, The Ohio State University The Syrian civil war has entered its fifth year with few signs of ending. The fighting has forced more than 13.5 million Syrians to flee their homes. Most of the displaced have not left Syria, but have simply moved around the country in an attempt to get out…
-

What’s Driving sub-Saharan Africa’s Malnutrition Problem?
Sub-Saharan Africa has the highest level of food insecurity in the world. An estimated 220 million people lack adequate nutrition. The nature of the problem is shifting rapidly, with overweight status and obesity emerging as new forms of food insecurity while malnutrition persists. But continental policy responses do not address this changing reality.
-

Fighting the Anti-Vaccine Rhetoric with Science
In the interest of promoting more robust discourse around the importance of regular vaccinations for serious but preventable contagious conditions, MHA@GW is hosting a guest post series in honor of National Immunization Awareness Month (NIAM). During the month of August,they’re featuring blogs from thought leaders and advocates who were asked to answer the question, “Why…
-

The Push to End Meningitis Cases and Outbreaks: MHA@GW Observes National Immunization Awareness Month
Featured photo: A child receives a meningitis vaccination at the Al Neem Camp for Internally Displaced Persons (IDPs) in El Daein, East Darfur, Sudan. UN Photo/Albert González Farran In the interest of promoting more robust discourse around the importance of regular vaccinations for serious but preventable contagious conditions, MHA@GW is hosting a guest post series…
