-

Donate to Help Expecting Mothers in Haiti
It is difficult to believe how much Haiti is suffering. Not only was its president assassinated a little over a month ago, but a 7.2 magnitude earthquake hit last weekend with a death toll now of over 1400. And, if that is not enough, a tropical storm is quickly barreling its way towards the island…
-

Impress Mom With These Maternal Health Mother’s Day Gift Ideas + Giveaway
Mother’s Day is the perfect holiday to splurge on the moms in your life as well as to support moms around the world. It’s a day to show love for mothers we know and to also remain mindful of the mothers everywhere who may need a little or even a lot of help for them…
-

Residents in Southern Haiti Receive New Access to Quality Health Care
During my visit to Haiti two years ago I had the privilege of visiting two hospitals: L’Hôpital Albert Schweitzer (HAS) in Haiti’s Artibonite Valley and L’Hôpital Sainte-Thérèse in Hinche, Haiti. Many of the patients at both hospitals, I learned, walked or took public transport over long distances for quality hospital care. As the poorest country in the…
-

Book Review: To Fool the Rain: Haiti’s Poor and Their Pathway to a Better Life
To Fool the Rain: Haiti’s Poor and Their Pathway to a Better Life by Steven Werlin My rating: 4 of 5 stars “Helping families lift themselves out of poverty means helping them build income and wealth, but it is a social phenomenon as well,” wrote Steve Werlin, the author of To Fool the Rain: Haiti’s…
-
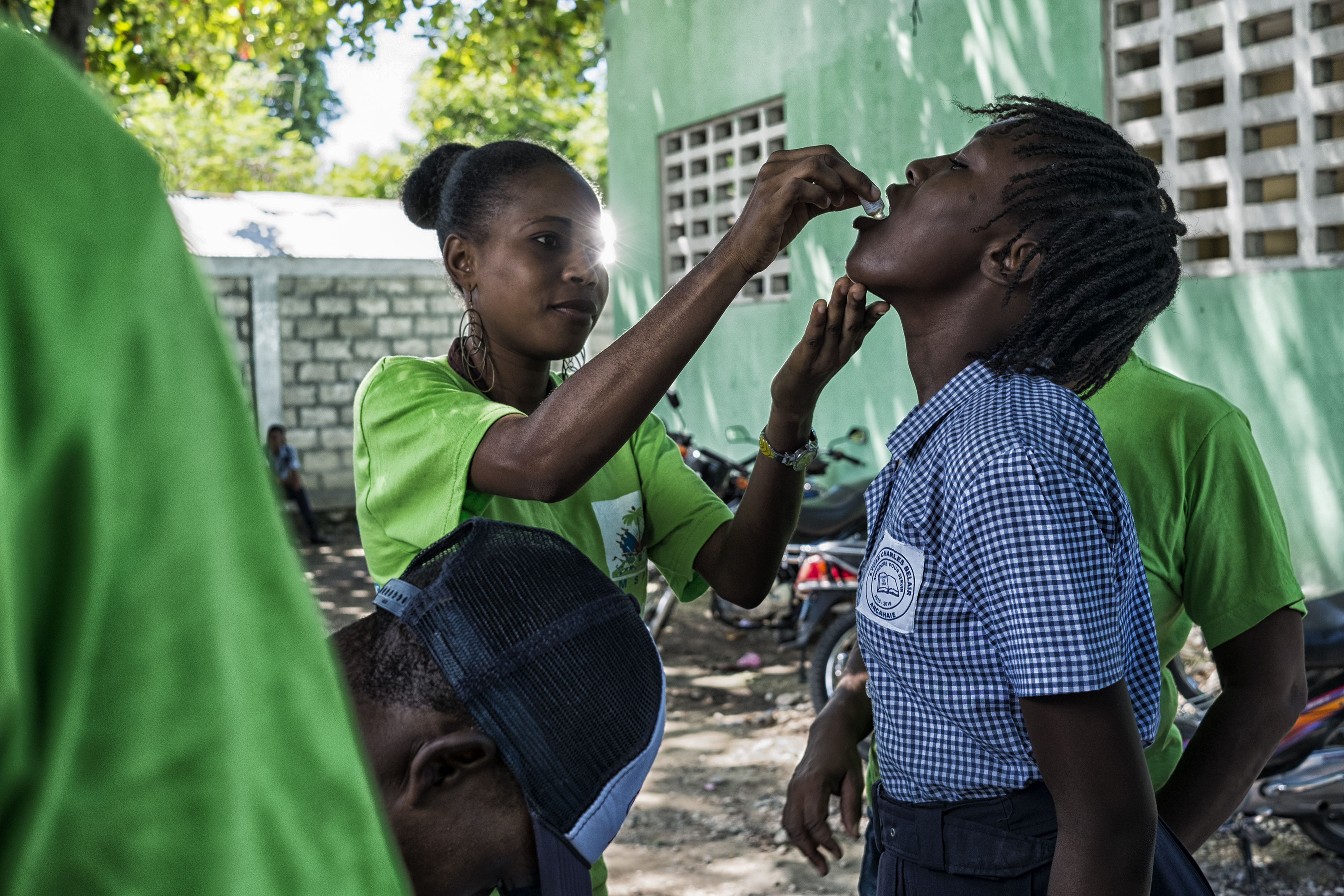
As the UN finally Admits Role in Haiti Cholera Outbreak – Here is How Victims Must be Compensated
Rosa Freedman, University of Reading and Nicolas Lemay-Hébert, University of Birmingham The United Nations has, at long last, accepted some responsibility that it played a part in a cholera epidemic that broke out in Haiti in 2010 and has since killed at least 9,200 people and infected nearly a million people. This is the first…
-
[Updated] Photographer Captures the Realities of Maternal Health in Haiti
B.D. Colen, a documentary photographer, is currently in Haiti with our partner Midwives for Haiti capturing the realities of maternal health for many Haitian women who live in the country’s poor Central Plateau. The mothers who receive care from Midwives for Haiti are the lucky ones. They have access to prenatal care at mobile clinics in…
-

Humanitarian Designs Innovative Diaper for Developing Countries
Michael Wahl didn’t purposely set out to create an innovative cloth diaper for babies who live in the developing world as well as a humanitarian organization, Dri Butts, that distributes diapers to families in need. Rather, he saw it as a necessity to prevent diseases caused by the spread of fecal matter. Many children in low-and middle-income…
-

Report – UN Peacekeepers Engage in Sex Exploitation in Haiti
While visiting Haiti you will see that the United Nations’ presence is palpable across the country especially in the capital Port-au-Prince where the United Nations Stabilization Mission in Haiti (MINUSTAH) is housed. During rush hour it is not uncommon to see countless UN vehicles with peacekeepers and leaders in berets (mostly men) among the many motos and cars…
-

Cervical Cancer: Haitian Women’s Next Biggest Killer
By Dr. Leslee Jaeger Roseline had delivered her baby during the chaos of our first day at Mama Baby Haiti, a birthing center for women near CapHaitian, Haiti. Mondays are the busiest day at the center, located on a dirt road just off Highway 1, as it is the intake day for expectant mothers that are…
-

Newborn and Child Health Education Through Haitian Art
Inside the child malnutrition unit at Hôpital Albert Schweitzer, the largest regional hospital in Haiti’s Artibonite region, colorful murals have been painted over the beds. They were specifically designed to teach parents, especially mothers, how to keep their newborns and children healthy and well-fed. In Haiti one in five children suffers from chronic malnutrition and…
-
![[Photos] Haiti Works Toward Eliminating Maternal Tetanus](https://socialgoodmoms.com/wp-content/uploads/2015/05/dsc8627.jpg)
[Photos] Haiti Works Toward Eliminating Maternal Tetanus
Casimer Dieuvela, 24 years old and five months pregnant, lives two to three hours walk from her monthly health post in Deschappelles, Haiti, but she goes despite the distance to receive her tetanus shot. It’s her third time coming to the health post run by health agent Junior Exanthus and arranged by Hôpital Albert Schweitzer (HAS). Dieuvela brings…
-

Infographic: 2015 Mothers’ Index Rankings
As in years past, the Nordic countries lead the world in being the best countries to be a mother and to raise children. Save the Children’s Mothers’ Index ranked countries based on maternal health, children’s well-being, educational status, and economic and political status. Sub-Saharan African countries and Haiti rounded out the worst places to be…
-

Maternity Ward Observations: Midwifery Care in a Haitian Hospital
The sunny, steaming hot morning when I visited L’Hôpital Sainte-Thérèse in Hinche, Haiti, the maternity unit was overflowing with busy midwives checking charts and administering care, nurses-in-training in white and yellow uniforms obtaining requisite clinical hours, as well as a few obstetricians checking on patients. Of course, there were expectant mothers, mothers who had just…
-
The Priceless Reaction of a Baby Being Vaccinated #Haiti
As I watched baby after baby receive the pentavalent (5-in-1) vaccine at a mobile health post put on by Hôpital Albert Schweitzer (HAS) in Haiti this week, their reactions were all the same. First, they were oblivious to what was going on. Then, they all felt a momentary prick of pain and the waterworks began.…
-
Health Agent Junior Exantus on Why He Became a Health Worker
Junior Exantus is a health agent for Hôpital Albert Schweitzer in Haiti. He has been a health agent for three years. “I wanted to enter the field to help the community,” said Exantus through translation. “I saw a lot of illnesses in the community.”
-
Reporting From Haiti This Week
This week I am traveling around Haiti reporting on global health issues that affect women and children. In fact, I am writing this post in the back of a SUV with my fixer and translator headed south of Port-au-Prince to visit Social Good Moms’ partner, Midwives for Haiti. In the poorest country in the Western…
-
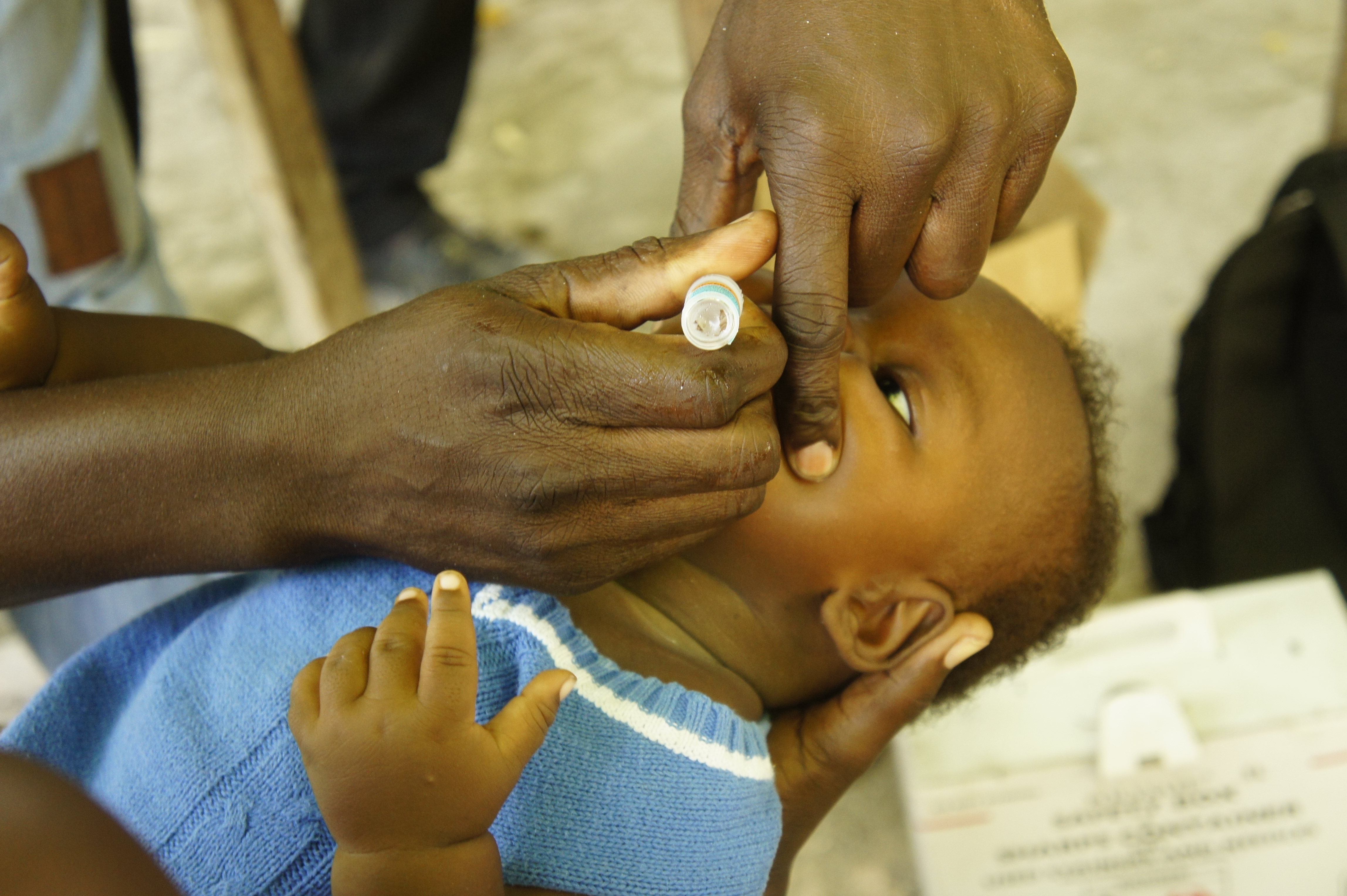
Photo Essay: Vaccines in Deschappelles, Haiti
Yesterday I was in Deschappelles, Haiti about three hours north of Port-au-Prince. Deschappelles is where the largest regional hospital, Hôpital Albert Schweitzer, is and has been for nearly 60 years. It serves a population of 350,000 and routinely takes in patients from outside of the region. In addition to hospital services Hôpital Albert Schweitzer also arranges and…
-

USAID Tackles Respectful Maternity Care, Better Working Conditions for Midwives
This week USAID released its follow-up to Ending Preventable Maternal Mortality: USAID Maternal Health Vision for Action (June 2014) with its new report of the same name with the addition of evidence for strategic approaches. These approaches seek to lower the world’s maternal mortality rate. Right now 289,000 women die per year from complications during…
-

5 of Our Partners Who Continue to Work in Haiti #Haiti5Years
In an earlier piece today, How is Haiti Faring Five Years After the Earthquake, development and recovery effort data and details were rather pessimistic. The numbers bear out that while some overall development achievements have been met, there is still a long way to go to help Haiti fully recover. And, yet, there continues to…
-
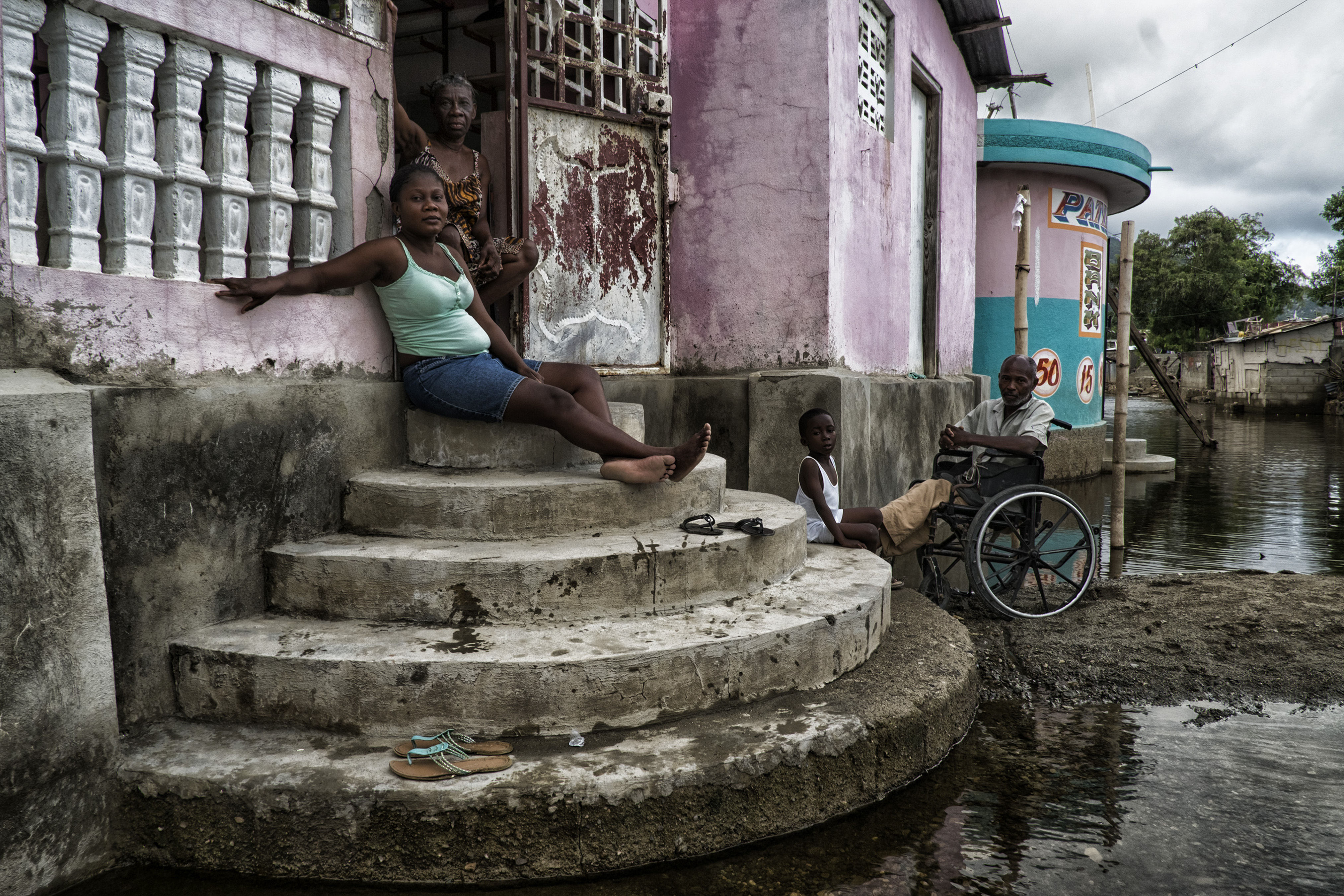
How Is Haiti Faring Five Years After the Earthquake?
Five years ago today, a magnitude 7.0 earthquake destroyed large regions of Haiti especially Port-au-Prince and Jacmel. For the poorest country in the western hemisphere, the earthquake only exacerbated poverty matters for its citizens and its standing in the world economy. An estimated 230,000 people lost their lives and 1.5 million more were displaced. Since 2010, $13…
