-

Arizona’s Now-Repealed Abortion Ban Serves As a Cautionary Tale For Reproductive Health Care Across the US
When the Arizona Supreme Court ruled on April 9, 2024, that the state’s Civil War-era law banning nearly all abortions was enforceable, it brought into stark reality the potential impacts of leaving reproductive rights up to the states to regulate, and the related consequences for women’s health.
-
Why sexual and reproductive law for east African countries is being resisted
Anthony Idowu Ajayi, African Population and Health Research Center and Nicholas Okapu Etyang, African Population and Health Research Center Six of the countries of the East African Community – Burundi, Kenya, Rwanda, South Sudan, Uganda and Tanzania – recently concluded public hearings on a new sexual and reproductive health bill. Proponents of the bill argue…
-
Kenya’s Marie Stopes ban may drive more women to unsafe abortions
According to the Kenya Medical Practitioners and Dentists Board, they banned abortion services provided by Marie Stopes following complaints from the general public. Restrictive laws mean that women resort to unsafe means. jbdodane/Flickr Michael Mutua, African Population and Health Research Center The Kenyan Medical Practitioners and Dentists Board has stopped the NGO Marie Stopes International from performing…
-
Why Family Planning Matters for Maternal Deaths and Child Survival
Contraception empowers women to plan the number of children they will have. Tizta Tilahun Degfie, African Population and Health Research Center Family planning improves child survival and reduces maternal deaths. But the uptake of family planning in Africa is only 33%, nearly half the world average of 64%. The contraceptive prevalence rate in African countries…
-
Will Trump’s Global Family Planning Cuts Cause Side Effects?
Actress and U.N. Population Fund Goodwill Ambassador Ashley Judd visited a refugee camp in Mafraq, Jordan in 2016. AP Photo/Raad Adayleh Written by Rachel Sullivan Robinson, American University School of International Service President Donald Trump is leading an assault on family planning around the world. Most recently, his administration cut off U.S. contributions to the…
-

Why The Global Gag Rule Will Increase Maternal Mortality
Throughout my visits to clinics in Africa I have seen the work of Marie Stopes International in South Africa, Tanzania, Ethiopia as well as Zambia. They provide a full range of quality reproductive health services for women. I have always been impressed by the comprehensive care they provide. Now, their work will be hampered because…
-

Better Maternal Care in Africa Can Save Women from Suffering in Childbirth
Kareemah Gamieldien, Cape Peninsula University of Technology Every year just over 500,000 women die from complications in pregnancy and childbirth across the world. Another 20 million experience severe complications. But many of these complications are entirely avoidable – including obstructed and protracted labour and one of its side-effects, obstetric fistula. An obstetric fistula is a…
-

Why Mothers Aren’t Accessing Antenatal Care Early in Their Pregnancies
Anja Smith, Stellenbosch University South Africa has extremely high maternal mortality levels. This is true when compared with developed countries as well as other developing countries. According to the World Health Organisation, for every 100,000 live births in the country in 2015, 138 women died due to pregnancy and childbirth complications. In Sweden, fewer than…
-

IN PHOTOS: Family Planning from Addis Ababa to Johannesburg
People the world over come here every day looking for family planning information. Knowing that, I have decided to create a compendium post of sorts about everything I have learned and seen about family planning in my travels to and reporting from sub-Saharan Africa over the past few years. I first learned about the critical importance of…
-

5 of Our Partners Who Continue to Work in Haiti #Haiti5Years
In an earlier piece today, How is Haiti Faring Five Years After the Earthquake, development and recovery effort data and details were rather pessimistic. The numbers bear out that while some overall development achievements have been met, there is still a long way to go to help Haiti fully recover. And, yet, there continues to…
-

Ethiopian Health Workers Receive Influx of Family Planning Training
In sub-Saharan Africa, 49 million women use traditional methods of family of no family planning methods at all. In Ethiopia, 39.1 percent of women use modern contraceptives up from 15 percent in 2005. The current low rate of contraceptive use in Ethiopia is a result of a combination of factors: cultural biases as well as a…
-

Our 12 Biggest Highlights of 2014
2014 was a very good year! We partnered with leading NGOs and nonprofits to advance causes that mean the difference between life and death and quality living for the world’s poorest citizens. We traveled around the world to report on water and sanitation, newborns, maternal health, disaster relief, and health workers. We traveled domestically to report…
-

Join Ashley Judd In Supporting Health Workers in Haiti
By Ashley Judd, PSI Global Ambassador Virgila is more charismatic and animated than most actors I know. She’s a PSI-trained health worker on the outskirts of Port Au Prince, Haiti. And she’s passionate about her work. She goes door-to-door educating women about the benefits of reversible contraception like the IUD. Giving birth is dangerous business…
-
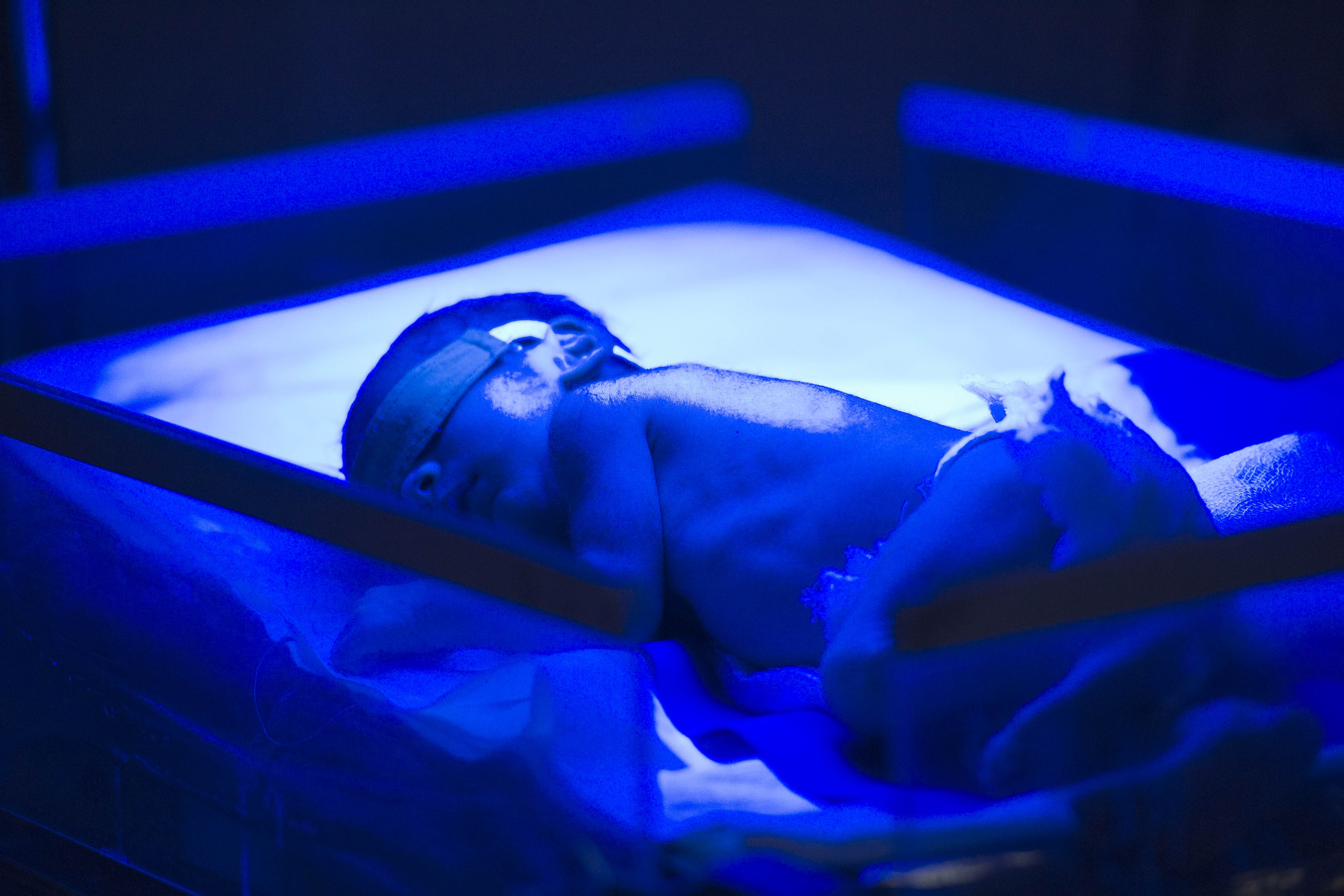
7 Facts About Premature Births You Might Not Have Known
Photo: A premature baby is shown in the postnatal ward at Cama Hospital, a major hospital for women and children, in Mumbai, India. UN Photo/Mark Garten Premature births are now the number one killer of babies globally. Of the 6.3 million children under five who died last year, 1.1 million of them died due to complications from premature…
-

How PSI Reinforces Positive Reproductive Health Messaging Through Branding, Edutainment
In Tanzania, orange has increasingly become the recognized color of family planning and reproductive health services. Population Services International’s orange Familia brand is quite common in most regions of this coastal country of 49 million. PSI, a global non-profit organization dedicated to improving the health of people in the developing world, has consistently and effectively…
-

A Day in the Life of a Family Planning Health Worker
Salasala, Tanzania — It took over an hour in notoriously congested Dar es Salaam traffic and gingerly moving through winding, narrow, dirt roads to visit Blandina Mpacha. Mama Blandina, as her community affectionately calls her, is a PSI health worker who teaches women, men, and whole families about the importance of family planning. This isn’t…
-

Traveling to Tanzania With PSI, IntraHealth International, and Mandy Moore
Over the years I have had the distinct privilege of meeting health workers around the world from Ethiopia and Kenya to Tanzania and South Africa to India and Brazil. Health workers, particularly in low- and middle-income countries, are the unequivocal backbone of health systems that can oftentimes be severely taxed due to the overwhelming number of people…
-

Uganda Holds First National Family Planning Conference
While her husband holds their youngest child, Twesigye Christente waits to receive a long-acting contraceptive at the Kinaaba Health Center II. Photo: UNFPA/Omar Gharzeddine This week Uganda held its first national family planning conference in Kampala. This is particularly significant because family planning has not always been pressing on the agenda of Uganda’s longtime president, Yoweri Museveni. In…
-
Journalists Travel to Ethiopia to Report on #NewbornHealth
It may seem a little quiet around SocialGoodMoms.com, but for good reason. I am co-leading a group of journalists throughout Ethiopia who are reporting on newborn health with the International Reporting Project. Putting together a robust itinerary for the journalists has been a capstone to all of the knowledge I have gained since learning about…
-

Rwanda Leads the World in Women Lawmakers
By Elaine Tucci Elaine Tucci is the Co-Founder and CEO of Women Lead to Change www.womenleadtochange.org As the world learns more about the promise of women to bring peace, prosperity and economic well-being to nations, Rwanda has become a poster child of this promise. Thriving after one of the most brutal genocides in history, today…
